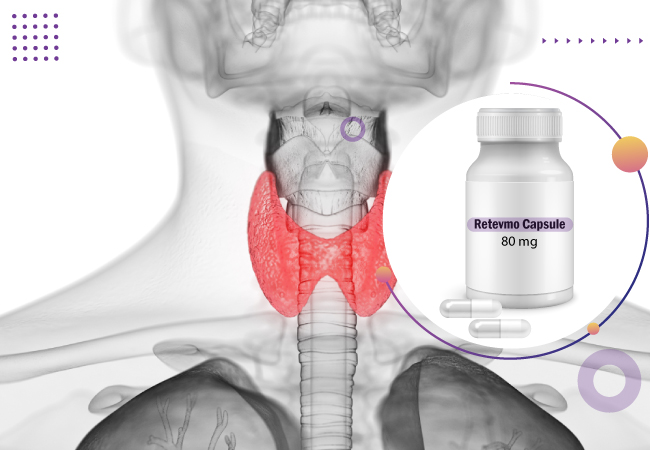
Thyroid cancer is one of the cancers that start in the thyroid gland. Cancer starts when cells begin to grow out of control. The thyroid gland makes hormones that help regulate your metabolism, heart rate, blood pressure, and body temperature.
The types of thyroid cancer are:
- Papillary thyroid cancer
- Follicular thyroid cancer
- Medullary cancer
- Anaplastic thyroid cancer
Medullary thyroid cancer, or MTC, is cancer that forms in the thyroid. The thyroid gland is present in the front of the neck, just below Adam’s apple. This gland is responsible for sending out hormones to the rest of the body. The inside of the thyroid gland is called the medulla. The medulla contains special cells, parafollicular C cells, that secrete and release hormones. MTC (Medullary thyroid cancer) occurs when the C cells become cancerous and grow uncontrollably
Symptoms of Medullary thyroid carcinoma
The common symptoms of Medullary thyroid carcinoma are:
- Neck lump
- Neck pain
- Hoarseness
- Coughing
- Trouble swallowing
- Shortness of breath
The other symptoms of Medullary thyroid carcinoma are:
- Severe diarrhea
- Cushing syndrome
- Facial flushing
- Bone pain
- Lethargy
- Weight loss
How is medullary thyroid cancer diagnosed?
The earlier medullary thyroid cancer (MTC) is found, the more likely it can be stopped and treated.
Imaging: Medullary thyroid cancer is diagnosed by the doctor first feeling your throat to check for a lump, continued by imaging scans of the thyroid. Imaging scans could include ultrasound, CT, or MRI.
Biopsy: The doctor will also want to take out a small amount of tissue, called a biopsy, from the thyroid. A pathologist will look at the tissue under the microscope to see if there are cancer cells and, if so, what type of thyroid cancer it is.
Treatment for MTC
The primary treatment for medullary thyroid carcinoma (MTC) is extensive and meticulous surgical resection. Both sporadic MTCs and FMTCs are treated with total thyroidectomy and lymphatic dissection of the anterior compartment of the neck.
Metastasis to the cervical lymph nodes is common in patients with MTC, particularly those with familial forms with multicentricity and bilaterality of the primary tumor. Lymph node metastases can occur in more than 50% of patients.
The first targeted therapy approved by the US FDA, Selpercatinib (Retevmo), is for tumors rearranging during transfection (RET) mutations. It is used for advanced or metastatic RET-mutant MTC in adults and children 12 years or older who require systemic therapy.
MTC is the most common cause of mortality in patients with MEN 2A and MEN 2B, and many patients who inherit these syndromes develop MTC in the first decade of life. Therefore, prophylactic thyroidectomy and central-compartment lymph-node dissection are performed in children with these syndromes.
Follow-up care
After receiving treatment for MTC, patients are monitored with an annual measurement of serum calcitonin levels for surveillance.
Radiation therapy is used in some centers in an adjuvant setting and can be used to treat patients with surgically inoperable recurrences and metastases. Because MTC does not concentrate iodine, radioiodine therapy has no role in follow-up care or treatment.
A variety of chemotherapeutic regimens have been used to treat metastatic disease.
Vandetanib (Caprelsa) and cabozantinib (Cometriq) are tyrosine kinase inhibitors approved by the FDA for progressive, metastatic medullary thyroid cancer.
Reference: https://emedicine.medscape.com/article/851968-overview#a7
https://www.cancer.gov/pediatric-adult-rare-tumor/rare-tumors/rare-endocrine-tumor/medullary-thyroid-cancer#:~:text=Medullary%20thyroid%20cancer%2C%20or%20MTC,thyroid%20is%20called%20the%20medulla.
https://www.healthline.com/health/medullary-thyroid-cancer/signs-and-symptoms